
7 Fertility Hormones That Regulate Female Reproductive Cycle
The female menstrual cycle runs like clockwork. Every month in a timed and synchronized manner the following events happen:
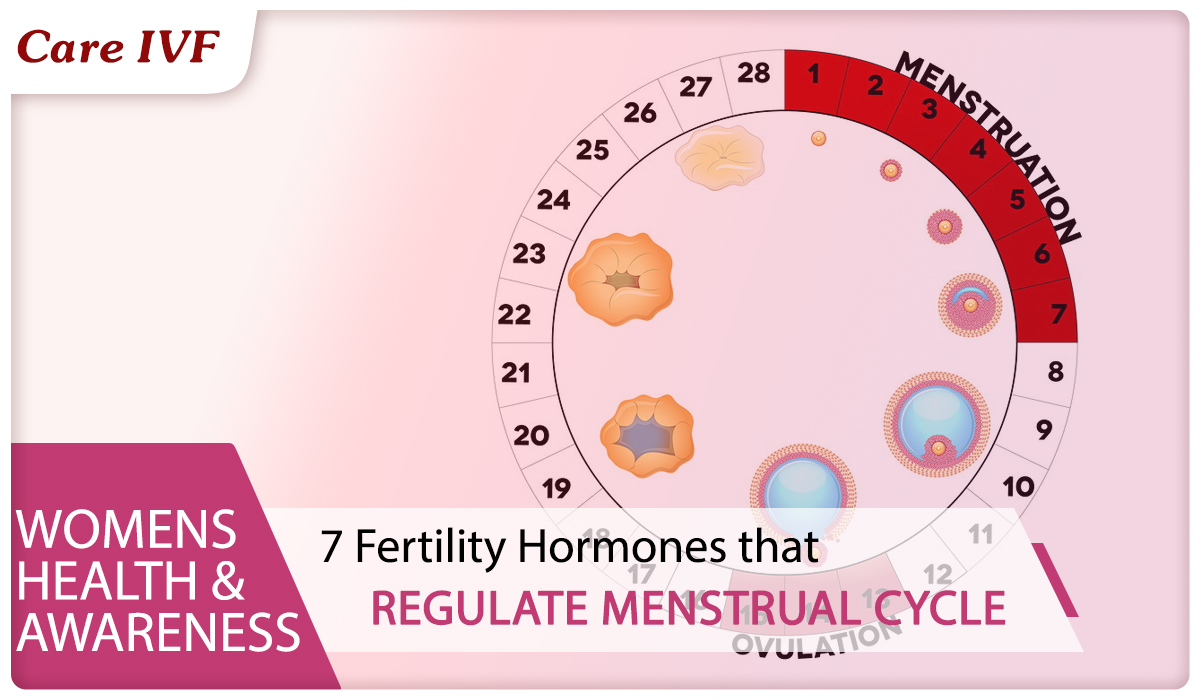
- A period of follicular growth starts in ovaries (follicles are fluid filled sacs that contain a growing egg), to release a mature egg. One egg is released per cycle from one of the ovaries.
- These follicles secrete the female hormone estrogen which is responsible for the growth of the uterine lining.
- The uterine lining undergoes thickening in preparation of the embryo
- If no implantation happens, the lining is shed and the cycle begins again
Not only does the body need make sure the physiological changes in the ovaries and uterus are taking place in cyclical manner but also ensure they occur in sync with each other. This utero- ovarian synchrony is very a important requisite for implantation success.
So how do the ovaries communicate to the uterus and vice versa?
How does your body maintain this monthly cycle and Utero-Ovarian synchronization?
It does so via hormones.
The Brain is the command centre that speaks to the reproductive organs via chemical messengers called hormones.
The menstrual cycle is kick started by the brain. There are two areas in the brain that regulate the female reproductive cycle that is Hypothalamus and Pituitary Gland
- Hypothalamus –this is located in the central part of the brain, and produces the hormone GnRH – Gonadotrophin Releasing Hormone. This hormone acts on the Pituitary Gland to release two GONADOTROPINS - FSH and LH.
- Pituitary gland – is about the size of a cherry and is located at the base of the brain behind the bridge of the nose.
Let us learn what these hormones that influence female fertility
PRE OVULATION:
GONADOTROPIN RELEASING HORMONE:
(Secreted by: Hypothalamus)
During the first few days of the ovulatory cycle, the hypothalamus produces gonadotropin releasing hormone (GnRH), which stimulates the pituitary to produce follicle stimulating hormone. Gonadotropin hormone-releasing hormone (GnRH) is the key regulator of the reproductive cycle.
FOLLICLE STIMULATING HORMONE (FSH)
(Secreted by: Pituitary Gland)
Is responsible for stimulating the ovaries to develop follicles (In men it stimulates sperm production). In the first few days of the menstrual cycle the FSH levels stimulates the development of a group of follicles in the ovary.
As the follicles develop they produce the hormones estradiol and inhibin that have an inhibitory effect on the the production of FSH, so that only the biggest follicle (dominant follicle) thatis competent enough to survive in the falling hormonal levels would grow to maturity.
An abnormally high FSH on Day 2 of the menstrual cycle can indicate declining ovarian reserve (low egg numbers). This may be checked with a blood test on Day 2 of your cycle, and the results should be discussed with your doctor/specialist.
ESTRADIOL
(Secreted by: Ovarian Follicles, Corpus luteum)
This hormone is produced by the granulosa cells (lining of the wall of follicle). Estradiol is a crucial hormone in the ovulatory cycle. The fluctuating levels of Estradiol controls when Endometrium is shed (menstruation), new endometrium grows and ovulation occurs.
- Estradiol is produced by the granulosa cells of the growing follicles. In the early phase of menstrual cycle, the levels are low. Low levels of Estradiol and Progesterone signals the shedding of endometrium
- As the follicle grows the estrogen rises and this rising estrogen levels causes a spike up the LH levels from the Pituitary gland. This rise in LH is called the LH surge and is responsible for the release of the mature egg.
- The rising levels of Estradiol and Progesterone prepares the lining of of the womb.
- The Estradiol in combination with another hormone called Inhibin acts on the hypothalamus and pituitary gland to reduce the production of FSH. Therefore Estradiol and Inhibin collaborate to act as regulators to regulate how much FSH is being produced throughout the cycle.
LH SURGE AND OVULATION
LH – LUTENIZING HORMONE
(Secreted by : Pituitary Gland)
LH secreted from the Pituitary Gland at low levels throughout the menstrual cycle. At the midpoint of the menstrual cycle, when estradiol reaches a threshold value, it induces a surge of luteinizing hormone, which stimulates the release of a mature egg.
POST OVULATION:
PROGESTERONE
(Secreted by : Ovarian follicles , Corpus luteum)
High levels of Estradiol and Progesterone = Endometrial growth and thickening
Following ovulation the Corpus luteum takes up the role of producing progesterone and there is a rise in its levels post ovulation. The post ovulatory follicle is now called the corpus luteum (Latin for Yellow Body). The corpus luteum produces both Estradiol AND PROGESTERONE, which are responsible for providing an environment in which the embryo can implant into the wall of the uterus and develop.
Low levels of Estradiol and Progesterone = Endometrial Shedding and Onset of menstruation
The corpus luteum has only a ‘life’ for 10-14 days, unless conception occurs. Towards the end of it’s lifespan the estrogen and progesterone levels drop. Which causes the lining of the uterus begins to break down, and marks the onset of menstrual bleeding.
INHIBIN
(Produced By: Growing follicles and Corpus Luteum)
Inhibin is secreted by the Corpus Luteum. Inhibin along with estradiol is the key inhibitor of FSH secretion. Basically, when Inhibin levels are low, FSH stimulates follicular recruitment and development in ovaries. FSH in presence of high levels inhibin (post ovulation) activates the signaling pathway that tells the brain (hypothalamus pituitary axis) to stop the production of FSH. So Inhibin together with both estradiol and progesterone secreted by the corpus luteum, accounts for the suppression of FSH and thus stopping the follicular development in the luteal phase of the human menstrual cycle. The drop in Inhibin at the end of cycle also causes rise in FSH productions that starts the next cycle.
IF CONCEPTION HAPPENS:
HUMAN CHORIONIC GONADOTROPHIN:
(Secreted by : Embryo, Placenta)
Successful implantation of embryo causes release of HCG (Human Chorionic Gonadotrophin) in to the blood stream which maintains the corpus luteum of pregnancy to provide hormonal support (estradiol and progesterone) to sustain the pregnancy.
About 7-8 weeks into pregnancy, Luteo – plancental shift occurs and the placenta takes over the making these hormones form the corpus luteum
This chart will help you understand the key hormones that control the Menstrual Cycles.
Don’t forget to read the following resources as well:
Understanding the Female Reproductive System
How to calculate the best days for trying to conceive?
Article Tags
About the author

Leave a Comment